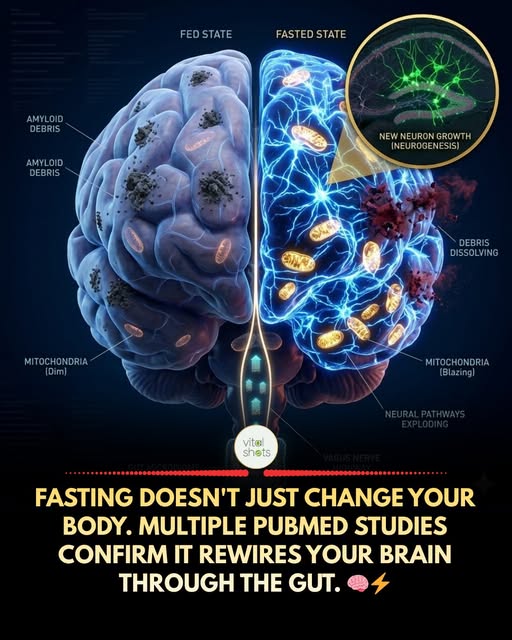
Most people try intermittent fasting because they want to lose weight. What they don’t realize is that some of the most compelling research on fasting has nothing to do with body fat.
It’s about what happens inside the skull.
A 2025 review published in PubMed (PMID:41356819) lays out the case in detail: intermittent fasting protects the brain through the gut-brain axis, not just through direct metabolic effects. When you fast, your gut microbiome composition shifts within days. Akkermansia muciniphila and other protective bacteria thrive during fasting windows. Short-chain fatty acids like butyrate rise. Intestinal barrier integrity improves. And from there, the brain feels it.
The mechanisms are specific. Fasting increases BDNF (brain-derived neurotrophic factor), often called “fertilizer for neurons,” which promotes hippocampal neurogenesis and synaptic plasticity. It reduces neuroinflammation via autophagy, a cellular “cleanup” process that clears damaged proteins including amyloid-beta, the same compound associated with Alzheimer’s progression. A separate 2025 paper (PMID:39798403) reviews evidence showing IF improves cognitive function in people with mild cognitive impairment, with the strongest mechanisms involving BDNF, CREB signaling, and reduced inflammatory cytokines in the brain.
One important nuance: duration matters significantly. Research from the gut-brain axis review indicates that short-term fasting protocols (around 8 weeks) are most effective at restoring gut barrier integrity and reducing systemic inflammation. Longer protocols (12+ weeks) begin to show more measurable effects on neurotrophic factors and actual cognitive performance. The two effects stack, which means consistency over time is more powerful than intensity in any single week.
The gut connection is what makes this genuinely new territory. For decades, fasting was studied almost entirely as a metabolic intervention. The idea that it works partly by growing better gut bacteria, which then signal the brain to repair and regenerate, reframes what we thought we understood about how lifestyle changes affect mental clarity, mood, and neurological resilience.
KEY FASTING PATTERNS STUDIED IN HUMANS
16:8 (16 hours fasting, 8 hours eating window) most common and sustainable protocol
5:2 (normal eating 5 days, very low calorie 2 days) studied specifically in older adults with insulin resistance (PMID:38901423)
Time-restricted eating aligned with morning light (earlier eating window) appears superior for circadian-based brain benefits
What does your current eating window look like? And have you ever noticed a difference in mental clarity or mood on days when you extended the fasting window?
Sources:
PMID:41356819 (IF and brain health via gut-brain axis, PubMed 2025).
PMID:39798403 (IF and neurocognitive disorders, PubMed 2025).
PMID:38901423 (IF in older adults with insulin resistance, PubMed 2024).
