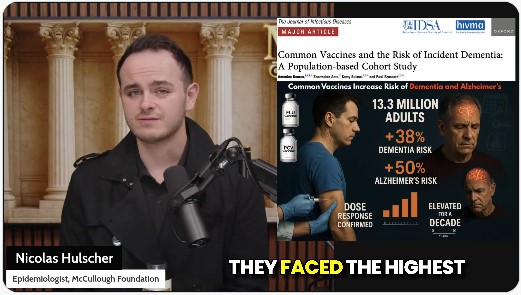
RFK Jr. called it a “trick”.
Dr. John Campbell called it “sly”.
Journals called it science.
just discussed one of the biggest scandals of our time with
which led to a “double whammy”. Dr. Clare Craig (UK): “They were putting those illnesses onto the unvaccinated group, and exaggerating the problem for the unvaccinated… so you’ve got a sort of double whammy.” Dr. Campbell: “Pretty sly trick really” And an Italian peer reviewed paper by Alessandria et al has now revealed how the “case counting window bias” meant that any deaths, hospitalizations, infections, or adverse events in that window were counted in the unvaccinated group. This “sly” statistical trick was used to sell “Pandemic of the Unvaccinated” and maintain the “safe and effective” narrative. Robert F Kennedy Jr. – “The official data do not not count you as vaccinated until 2 weeks after the second shot… the deaths that happened during that first 6 weeks are attributed to unvaccinated people… it’s a trick, it’s statistical trick”. Legacy media still hasn’t covered this scandal.