
You Have Rights


Tom's Blog on Life and Livingness

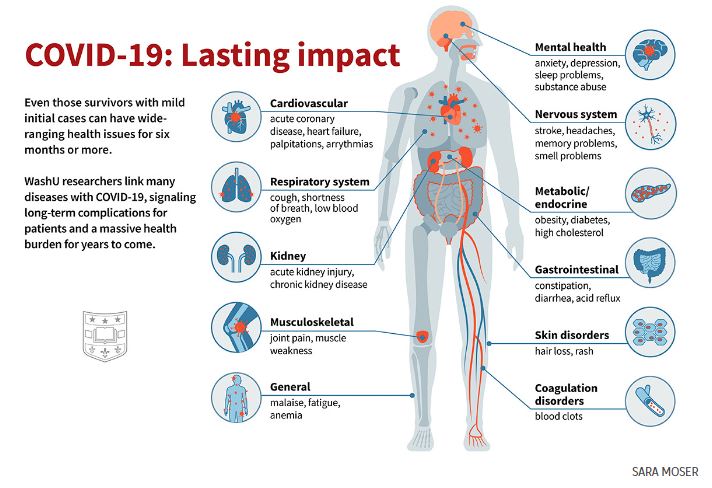
Among COVID-19 survivors, an increased risk of death, serious illness
https://medicine.washu.edu/news/among-covid-19-survivors-an-increased-risk-of-death-serious-illness/
I recently saw a report of a study that found 70% of long Covid sufferers had never had Covid, they had only received the jab.
To aid those tricked/coerced into getting the jab as well as those suffering from symptoms of shedding after being exposed to the jabbed, I have done my best to compile a Jab Recovery Protocol from the various sources I have seen: https://www.tomgrimshaw.com/tomsblog/?p=35644
And this is my attempt to assist those who don’t feel up to sourcing and compiling the ingredients themselves:
https://www.healthelicious.com.au/NutriBlast-Anti-Spike.html

Anecdotes include that of a man who escaped Germany with only one suitcase, planning to return in a few days, after people who supported Hitler regained their sanity and ousted him. Another concerns a man who eventually gave in to his son’s persistent requests to be permitted to join the Nazi Party. He felt that by doing so, his son at least would avoid persecution by the brown-shirted minions of the regime. In doing so, he handed his son over to doom. It is questionable whether father or son survived the resulting war, the war that skeletonized Berlin and left its people starving, entirely reliant on the mercies of those whom they had, until then, tormented.
Key to all of this in the 1930s was the false perception, renewed each day, that the Nazi government had gotten so bad that matters could not possibly get any worse. They just had to turn around and get back to a normal, civilized society. After all, just how bad could things get? Could they possibly lead to a worldwide war? (Japan’s Pacific ambitions relied heavily on, and were encouraged by, the expectation that Germany would defeat the British Empire and thereby expel it from Asia.) And the idea of millions dying in “death camps” seemed preposterous in 1933. Only barbarians could enact such a policy. Surely, civilized Germany could never, ever do such a thing.
Is it fair to compare modern America to the Germany of the era of 1933–45?
Decide for yourself. In America, the so-called “Free Speech” movement of the 1960s quickly morphed into the practice of censorship by shouting down speakers with whom the left disagrees. How far can that get? Racial civil rights, a good thing, eventually was deceptively adapted to women’s rights, gay rights, and even “animal rights.” Women’s rights became the right to kill millions of unborn children. Racial civil rights became the debilitations of multi-generational welfare for life. Add to all these the right of criminals, even murderers, to be released without punishment. Okay, no farther.
But farther there was.
The right of gays to be “left alone,” and then to marry each other, eventually became the right of homosexuality advocates to teach small schoolchildren the sexual practices of sodomy. No, this can’t be true! No one could have foreseen that a president of the United States, abetted by the entire Democrat party, and the courts, would use taxpayer money to bring children into “sex change” clinics to mutilate them, to permanently destroy their ability to grow into their natural sex. One would have been deemed insane to predict such a thing.
We have in the Oval Office an increasingly senile puppet whose handlers not only permit millions of illegal aliens to flood our nation, swelling our census with future representatives who will represent them, not us — not only permit, but actually pay for their lawless border-crossing with our tax dollars.
We now have in Congress people who openly acquiesce to foreign powers sworn to destroy America. We have corporate boards of directors who despise the ordinary hardworking citizen and who openly sneer at our flag and ridicule the idea of selfless patriotism. The rot has so deeply infested our nation that at least one congressman has admitted that there is no normal, procedural way to set things right.
We used to trust that election officials would not rig elections.
For decades, the question has been asked: when will Americans wake up? They have yet to do so, and the nightmare not only continues, but gets worse. Just as in 1933 Germany, antisemitism has become a dreadful fact of the political scene, especially on American college campuses. How far will it go?
Unlike in twentieth-century Germany, there are a few people in power who recognize, and oppose, the present trend toward an American tyranny. Governor Abbott of Texas is one, and he has the explicit support of twenty-five other governors. We have a tradition of independence, of private weapons ownership, and of refusing to be silenced.
Will these few, citizens and governors, be enough? Or will we sink into the mire that swallowed the mighty epitome of civilization that Germany once had been? There will be no one to come to our aid — only foreign armies to trample us. Will we allow our children to be enslaved?
As President Reagan once said, there are no easy choices, but there are simple ones.
https://www.americanthinker.com/blog/2024/03/maybe_they_really_are_nazis_after_all.html

As I see it this intentional destruction, done with full complicity of the infiltrated Federal institutions, is best countered by the ordinary man and woman in the street starting at the local level to reclaim control over their school boards, local councils then building momentum from there to state governments and institutions that can nullify unconstitutional Federal regulations.
If you want to save The US of A, better start now! Get some mates together and strategise how you will take back your street, your suburb/town/city and state from the uniparty representatives that do not serve your interests.
We know that excess carbs like sugar and white flour can make us gain weight, but there are other culprits lurking in the food supply.
Recently the Washington Post published a puff piece on monosodium glutamate (MSG), claiming that we have nothing to fear from the artificial flavoring that adds umami “spark” to many dishes. The author, Aaron Hutchinson, marginalizes headaches and allergic reactions as minor symptom in a few hypersensitive people. Says Hutchinson:
“In addition to soup and eggs, MSG can be added to salad dressings, bread, tomato sauce, meats, popcorn, ‘an absolutely filthy martini,’ you name it. MSG is a great way to add flavor to just about anything except sweets. It’s particularly great with vegetables, too.”
He makes no mention of the real problem with MSG: weight gain. If you search “msg-induced obesity” at PubMed, you will come up with almost one hundred citations. It’s hard to get research animals to overeat and become obese — in order to study obesity — so scientists feed the rats, mice and hamsters MSG to make them eat more and put on weight.
Most of the citations are animal studies, not human trials, and the food industry has argued that the amount of MSG given to the animals is way more, as a function of body weight, than humans would ever eat. Or, they say, the association with weight gain and MSG is really an association of weight gain and processed foods, since MSG is in almost all processed foods.
What happens when we consume small amounts of MSG as a flavoring day after day after day? A 2008 study1 published in the journal Obesity provides confirmation that MSG indeed causes weight gain in humans, and not because of its inclusion in processed foods.
In this well-designed trial, researchers at the University of North Carolina at Chapel Hill studied 750 Chinese men and women, ages 40-59, living in three rural Chinese villages. Most of the study subjects prepared their meals at home without commercial processed foods and about 82% used MSG.
Those participants who used the highest amounts of MSG had nearly three times the incidence of overweight as those who did not use MSG, even when physical activity and caloric intake were accounted for.
What about the argument that the glutamic acid in MSG is the same as the essential amino acid glutamic acid that we get from protein foods? According to the Washington Post article, “The glutamate in MSG is chemically indistinguishable from glutamate present in food proteins. Our bodies ultimately metabolize both sources of glutamate in the same way.” The first sentence is true but the second sentence is false.
The glutamic acid in foods like meat is attached to various peptides and other compounds that release it when required and prevent it from overstimulating the nervous and endocrine systems; while the glutamic acid in MSG is “naked,” highly reactive and unmitigated by its milieu.
Americans consumed about one million pounds of MSG in 1950; today that number is three-hundred million pounds. Almost all processed and fast food contains MSG2 (usually not labeled), and the food industry certainly knows that the additive they use to make their food taste good is a major cause of the current obesity epidemic. The message to consumers is clear: to lose weight, it’s important to avoid all processed food, and certainly not add it to the foods you prepare at home.
As I have never met a diet soda-drinker who is slim, the results of a review study by Susie Swithers, Purdue University professor of psychological sciences and a behavioral neuroscientist, do not surprise me. Swithers found that consumption of diet soft drinks increases the likelihood of overeating.
One large study found that people who drink artificially sweetened sodas are more likely to experience weight gain than those who drink non-diet sodas. Other studies3 found that those who drink diet sodas have twice the risk of developing metabolic syndrome, often a precursor to cardiovascular disease, than those who abstained.
Use of diet sodas, sweetened with non-caloric sweeteners such as aspartame, sucralose and saccharin, has increased enormously over the last twenty-five years, as consumers try to steer clear of sugar and high fructose corn syrup. About 30% of American adults regularly consume these artificial sweeteners. What to drink if you need to watch your weight?
Try sour kombucha made with organic cane sugar — look for kombucha with less than 5 grams of sugar per serving. Or, make your own, letting it brew a long time (see my blog post “Kombucha Like Fine Champagne”4). Sparkling water with a squeeze of lemon and pinch of unrefined salt makes a refreshing and healthy soft drink. Herbal tea and bone broth are additional choices.
When it comes to weight loss, not all fats and oils are the same. Many studies have shown that saturated animal fats are far less likely to cause weight gain than polyunsaturated vegetable oils.
For example, one study5 found that mice fed excessive corn oil had increased caloric intake and obesity. In another,6 rats were divided into different groups receiving diets with identical proportions of calories from fat, protein, and carbohydrate but different types of fats.
The rats in the group receiving fat from safflower oil had a 12.3% increase in total body weight compared to the rats eating traditional fats. Weight gain was lower in the rats fed a higher proportion of saturated fats. For the average human, a 12.3% increase in total body weight translates into 23 pounds.
Vegetable oils that have been heated are even more obesogenic. In a randomized trial on rabbits,7 three groups of rabbits were given access to identical foods, with only one difference: the first group of rabbits was fed unheated vegetable oil, the second group was fed vegetable oil that had been heated once, and the third group was fed vegetable oil that had been repeatedly heated multiple times — as happens in deep friers. Everything else about their diets was kept the same.
The surprising outcome was that compared to the group of rabbits eating unheated oil, the group eating single heated oil gained 6% more weight, and the group eating repeatedly heated oil gained 45% more weight — even though the rabbits eating heated oil actually consumed a slightly lower level of calories. It seems that foods fried in vegetable oil are dieters’ worst enemy. Why would polyunsaturated vegetable oils cause weight gain? As explained by Jeff Nobbs:8
“When we eat a diet high in polyunsaturated fatty acids, omega-6s and or linoleic acid, over time, this leads to mitochondrial dysfunction, primarily with our electron transport chain. And the ETC is a very important process that creates ATP or energy … if these processes become dysfunctional, this is really bad, because what happens is we can’t effectively or properly burn fat as fuel.
Another thing that we start to see is reduced fatty acid beta oxidation which also means that we become less efficient at using fat as fuel and as a result we begin to prioritize carbohydrates as fuel … we are consuming high amounts of vegetable oils, we become less efficient at using fat as energy, while also making our fat cells bigger and grow in size, which is exactly what we don’t want and this could be a huge reason why we’re gaining weight and why it’s so difficult for us to lose weight!”
Dieters are often reluctant to embrace saturated animal fats, believing the propaganda that butter and lard will make you fat. But the science suggests otherwise. For example, a study9 by Temple University School of Medicine provides welcome vindication for Atkins and other practitioners who insist that the best way to lose weight is to eat a lot of fat — animal fat.
The study took place in a clinical research center where every calorie eaten and spent was measured. After a week of typical eating, 10 obese patients with Type 2 diabetes followed a diet that limited carbohydrates to 20 grams per day but allowed unlimited protein and fat.
With carbs out of the diet, the patients spontaneously reduced their daily energy consumption by 1,000 calories per day. “When carbohydrates were restricted,” said lead researcher Guenther Boden, MD, “the subjects spontaneously reduced their caloric intake to a level appropriate for their height, did not compensate by eating more protein or fat, and lost weight. We concluded that excessive overeating had been fueled by carbohydrates.”
In addition to calorie reduction and weight loss, subjects experienced markedly improved glucose levels and insulin sensitivity as well as lower triglycerides and cholesterol. The interesting thing about this study was that the subjects did not consciously try to restrict calories or lose weight, showing that restricting carbs and increasing fat in the diet works better than will power.
In yet another defeat for the low fat, you-must-suffer-to-lose-weight school of thought, a Swedish study10 has found that women who regularly consume at least one serving of full-fat dairy every day gained about 30% less weight than women who didn’t.
The researchers, from the Karolinska Institute in Stockholm, looked at the intake of whole, sour, medium- and low-fat milk, as well as cheese and butter for almost twenty-thousand Swedish women aged 40-55 years old — the age when most women should and do gain weight … but not too much.
The researchers reported that a regular and constant intake of whole milk, sour milk and cheese was significantly and inversely associated with weight gain (that is, those consuming whole-milk products did not gain much weight), compared to the other groups.
A constant intake of at least one daily serving of whole and sour milk was associated with 15% less weight gain, while cheese was associated with 30% less weight gain.
Two other studies have concluded that the consumption of whole fat dairy products is linked to reduced body fat. In one paper,11 middle aged men who consumed high-fat milk, butter and cream were significantly less likely to become obese over a period of 12 years compared to men who never or rarely ate high-fat dairy.
The second study12 is a meta-analysis of sixteen observational studies aimed at exploring the hypothesis that high-fat dairy foods contribute to obesity and heart disease risk. The researchers concluded that the evidence does not support this hypothesis; in fact, the reviewers found that in most of the studies, high-fat dairy consumption was associated with a lower risk of obesity.
The tragic practice of feeding reduced-fat milk to growing children, even prohibiting full-fat milk in schools and day care centers, in order to prevent weight gain, has no basis in science, as shown in a study13 from Canada.
Researchers followed over 2,700 children, ages 1 to 6. Children who got full-fat milk had a lower body mass index and also higher vitamin D status. Children who drank full-fat milk were less likely to end up hungry, and less likely to snack on high-calorie foods, suggested the researchers.
In U.S. schools, children have a choice of low-fat milk, which they hate, or chocolate milk made with skim milk powder and high fructose corn syrup — often containing almost as much sweetener as sodas! The message is clear: for weight loss, avoid all industrial seed oils and enjoy animal fats and full-fat dairy foods.
When you eat too much salt, you become thirsty and drink water so as to dilute the amount of sodium chloride in the bloodstream, keeping sodium at the proper levels and excreting the excess. This is the conventional view of the “salt equation.”
But experiments with mice found that mice burned more calories when they got more salt, eating 25% more just to maintain their weight. It seems that salt stimulates the production of more glucocorticoid hormones, which break down fat and muscle in the body.
In addition, salt-detecting neurons in the mouth control the urge to drink, and more salt results in a lower sensation of thirst. “The work suggests that we really do not understand the effect of sodium chloride on the body,” said a study author.14 “These effects may be far more complex and far-reaching than the relatively simple laws that dictate movement of fluid, based on pressures and particles.”
These results suggest that increasing salt may be a useful strategy for weight loss, as long as the diet contains sufficient levels of fat to mitigate increased feelings of hunger. The results also show the folly of the recent FDA push15 to get the food industry to lower salt content in processed foods.
The food industry isn’t complaining because they now have an additive they can use to make low-salt foods taste saltier: it’s called Senomyx. Senomyx and other flavor enhancers stimulate your taste buds without them actually tasting anything. Much like MSG, these flavor enhancers operate on the neurological level to produce these reactions.
Since they are not actually ingredients but rather “enhancers,” FDA does not require manufacturers to list them in the ingredients panel except as “artificial flavors.” Because very small amounts of the additives are used, Senomyx’s chemicals have not undergone the FDA’s usual safety approval process for food additives.
In fact, they are not flavors at all. They are chemicals that contain no flavor of their own, rather they activate or block taste receptors in your mouth. The chemicals can mimic or enhance the taste not only of salt, but also sugar and monosodium glutamate (MSG).
Already the industry is adding Senomyx to a huge number of products, from soups to coffee (for a salty taste) and from sodas to candies (for a sweet taste).16 So what could possibly go wrong?
Here’s one thing: your body has an absolute requirement for salt and if we don’t get the salt we need in our food, we just might eat and eat and eat salty-tasting foods in order to get the salt we need. Sounds like a great recipe for weight gain.
Those who write about the worldwide obesity epidemic have focused almost exclusively on life style issues such as consumption of high-calorie junk food and decreases in exercise. These remain plausible interpretations and are certainly contributing factors.
But new research opens up an entirely new theory — the disruption of weight regulation by hormone-disrupting contaminants. Japanese researchers17 have found that exposure to bisphenol A (BPA) in combination with insulin increases the number of fat cells in mouse cell tissue culture, and also causes the enlargement of fat cells.
Human exposure is widespread through consumption of water in plastic bottles. (Other sources are dental sealants, used on children’s teeth to “prevent cavities,” and foods packaged in plastic.)
Dr. Barry Durrant-Peatfield of the UK has also proposed the theory that even drinking water from the tap can make you fat — fluoridated water, that is. “There is no doubt that fluoride is enzyme disruptive and one thing it affects is thyroid hormones. As a result of this disruption, people can finish up with partial under-activity of the thyroid gland.”
According to Dr. Durrant-Peatfield, fluorine can replace iodine in the body, leading to thyroid problems and weight gain. He believes that children may be particularly susceptible to obesity if their mothers drank fluoridated water while pregnant.
He notes that UK obesity levels are highest in the West Midlands, the only area in England now fluoridated (Sunday Mercury, July 11, 2004). Yes, lots of compounds that make us gain weight are lurking in the food supply! If you want to lose weight, the very first assignment is to avoid them like the plague.
Sally Fallon Morell is author of the best-selling cookbook Nourishing Traditions and many other books on diet and health. She is the founding president of the Weston A. Price Foundation (westonaprice.org) and a founder of A Campaign for Real Milk (realmilk.com). Visit her blog at nourishingtraditions.com.
Article copied from Dr Joseph Mercola web site.

Mark Farnell writes: Feeling sad at the news of a friend and fellow researcher’s unexpected death (I reckon they bumped her off tbh, her exposes were that good). In honour of Tracey, I can do no better than plug her last book- it’s a fantastic read. Her memory will live on in her work.

You may have heard about how bad vegetable oils are by now. But have you ever wondered why? My biggest beef with vegetable oils is that they negatively impact your metabolic rate and gut health — the two most important factors that impact your state of health.
So, yah. It’s kind of a big deal that our food system is centered around them. And that mainstream nutrition advice from Harvard still recommends vegetable oil as a “healthy fat” because it lowers serum cholesterol.
But what about the well-known fact that PUFAs (polyunsaturated fats) are very unstable molecules? (And vegetable oils are high in PUFAs, specifically linoleic acid, an omega-6).
“Polyunsaturated fatty acids (PUFAs) are highly susceptible to lipid per oxidation because of their unstable double bonds.1
PUFAs, in this sense, are like delicate glass … When glass shatters, it invariably leaves behind a mess of dangerous shards … Likewise, when PUFAs shatter they leave behind shards such as MDA, which are capable of damaging proteins, DNA and other structurally and functionally important components of our cells.” ~ Chris Masterjohn, Ph.D.2
Having more of these fats around creates a damaging internal environment in your body. Thus, there are long term negative health consequences with high PUFA consumption. Let’s discuss a few of these consequences.
First, vegetable oils wreak havoc on the gut by increasing tight junction permeability.3 Tight junctions play an important role in intestinal barrier function by maintaining selective permeability. Well, unfortunately, PUFAs can increase the permeability of tight junctions. (Not what we want!)
In one study, the omega-6 PUFA rich diet increased host inflammation, oxidative stress, and gut barrier dysfunction:4
“The corn oil diet, rich in omega-6 polyunsaturated fatty acids, increased the potential for pathobiont survival and invasion in an inflamed, oxidized and damaged gut while saturated fatty acids promoted compensatory inflammatory responses involved in tissue healing.
We conclude that various lipids uniquely alter the host-microbe interaction in the gut. While high-fat consumption has a distinct impact on the gut microbiota, the type of fatty acids alters the relative microbial abundances and predicted functions. These results support that the type of fat are key to understanding the biological effects of high-fat diets on gut health.”
Okay so I will just up my omega-3s, the healthy PUFAs, right? Ehh, not so fast. High dietary omega-6 PUFA consumption has been shown to shift the gut microbiome and can induce gut dysbiosis and inflammation.5
But the authors of this study point out that while omega-3 PUFAs may lead to short-term inflammation reduction, this was due to immune suppression, which eventually led to other health problems and increased mortality.
Saturated fats are stable molecules and are protective. Unsaturated fats are unstable and can cause a lot of damage when consumed in excess. So, it makes sense why the gut can be damaged in the long run with high PUFA consumption.
“Clinically, excessive ω-6 polyunsaturated fatty acid (PUFA) and inadequate ω-3 PUFA have been associated with enhanced risks for developing ulcerative colitis. In rodent models, ω-3 PUFAs have been shown to either attenuate or exacerbate colitis in different studies.
We hypothesized that a high ω-6: ω-3 PUFA ratio would increase colitis susceptibility through the microbe-immunity nexus. To address this, we fed post-weaned mice diets rich in ω-6 PUFA (corn oil) and diets supplemented with ω-3 PUFA (corn oil + fish oil) for 5 weeks. We evaluated the intestinal microbiota, induced colitis with Citrobacter rodentium and followed disease progression.
We found that ω-6 PUFA enriched the microbiota with Enterobacteriaceae, Segmented Filamentous Bacteria and Clostridia spp., all known to induce inflammation. During infection-induced colitis, ω-6 PUFA fed mice had exacerbated intestinal damage, immune cell infiltration, prostaglandin E2 expression and C. rodentium translocation across the intestinal mucosae.
Addition of ω-3 PUFA on a high ω-6 PUFA diet, reversed inflammatory-inducing microbial blooms and enriched beneficial microbes like Lactobacillus and Bifidobacteria, reduced immune cell infiltration and impaired cytokine/chemokine induction during infection.
While, ω-3 PUFA supplementation protected against severe colitis, these mice suffered greater mortality associated with sepsis-related serum factors such as LPS binding protein, IL-15 and TNF-α. These mice also demonstrated decreased expression of intestinal alkaline phosphatase and an inability to dephosphorylate LPS.
Thus, the colonic microbiota is altered differentially through varying PUFA composition, conferring altered susceptibility to colitis. Overall, ω-6 PUFA enriches pro-inflammatory microbes and augments colitis; but prevents infection-induced systemic inflammation.
In contrast, ω-3 PUFA supplementation reverses the effects of the ω-6 PUFA diet but impairs infection-induced responses resulting in sepsis. We conclude that as an anti-inflammatory agent, ω-3 PUFA supplementation during infection may prove detrimental when host inflammatory responses are critical for survival.”6
PUFAs Negatively Impact Thyroid and Metabolic Health
Another consequence of high PUFA consumption is that PUFAs can negatively impact thyroid and metabolic health since they interfere with your cell’s ability to utilize active thyroid hormone. It’s great that our body can convert T4 to active T3. But to increase energy production, our cells must be able to access that T3.
In fact, tissue T3 levels are different than serum T3,7 which is why one of the best ways to assess metabolic and thyroid health is through body temperature and pulse measurements (which I discuss in depth here), since higher cellular T3 increases the metabolic rate, raises body temperature, and increases our pulse.8 Understanding this helps us realize why it’s a bad thing that PUFAs interfere with your cell’s ability to use active thyroid hormone, T3.
“Safflower oil [high in Omega-6 PUFA] was more effective than tallow as a repressor of T3 action … polyunsaturated fats uniquely suppress the gene expression of lipogenic enzymes by functioning as competitive inhibitors of T3 action, possibly at the nuclear receptor level.9
The potency of unsaturated fatty acids for INB (Inhibition of Nuclear T3 Binding) was greater than of saturated fatty acids, and increased with the number of double bonds.10
The effects of selected fatty acids (linoleic – PUFA, oleic – MUFA, and palmitic – SFA) on triiodothyronine (T3)-receptor binding were compared … the rank order of potency for inhibition was linoleic acid greater than oleic acid greater than palmitic acid.”11
It’s never about extremes. You cannot eat a zero PUFA diet and that is not the goal. But you do not need to over consume PUFAs. You do not need to add more omega-3s to your diet if you are consuming animal fats. You do not need to add fish oils, you do not need to force flax seeds down your throat. And you certainly don’t need to increase your vegetable oil consumption.
Instead, eat real, whole foods. And for your fats, prioritize animal fats that are rich in the stable, protective saturated fats. Just like your great grandma. This will provide your body with more of an optimal fatty acid profile without over thinking it. Plus, this approach just makes sense.
Vegetable oils did not exist 100 years ago. People did not force fish oils down their throat. They enjoyed a diet rich in animal products, and consumed saturated fat without fear. And the rates of autoimmune and chronic diseases we face today was certainly not as high.
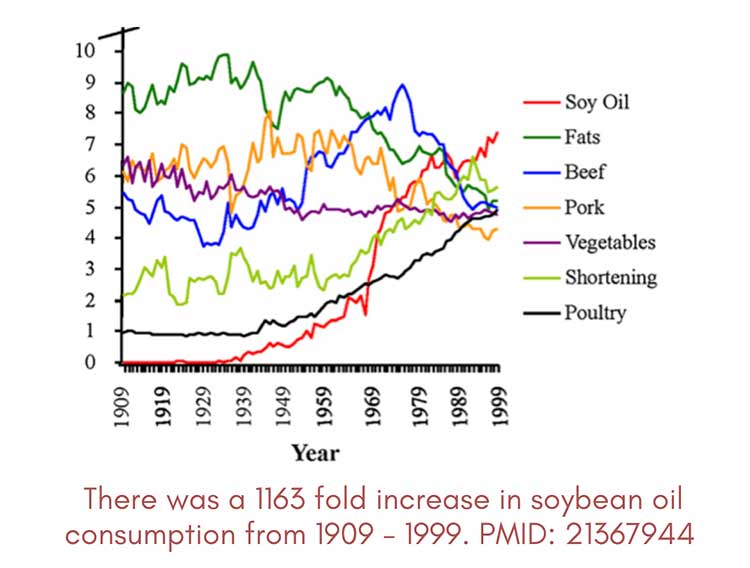
What your food eats, matters — as pigs and chickens are vehicles for vegetable oils. (So if their diet is high in PUFAs, the final product will contain more PUFAs). With the current agriculture system, knowing where your food comes from is vital. The article was written by Ashley Armstrong, who is passionate about providing the highest quality food possible.
Armstrong is the cofounder of Angel Acres Egg Co., which specializes in low-PUFA (polyunsaturated fat) eggs. We discussed the importance of low-PUFA eggs in a recent interview, embedded above for your convenience.
Angel Acres Egg Co. ships Low PUFA eggs to all 50 states — but there is currently a waiting list as she slowly increases the number of chickens within the network to fulfill the demand. More egg boxes will be available this spring — join the waitlist for low PUFA egg boxes here.
Armstrong also co-founded Nourish Cooperative which ships the best low PUFA pork, beef, cheese & A2 dairy and traditional sourdough to all 50 states. They are also close to accepting new members to the farm cooperative — join the waitlist here: nourishcooperative.com.
In the video segment above Ashley reflects on the timeline of her decision to invest her free time into regenerative farming. Considering how just a few years ago, her health was far from ideal. She struggled with mitochondrial energy production, and her body was in a low thyroid state. Your body prioritizes energy for essential tasks, and decision-making requires significant energy.
Your brain consumes about 20% of your body’s energy despite being only 2% of its weight. Ashley simply would not have had enough cellular energy to supply her brain to make a decision like she did unless she improved her health. Factors like excess linoleic acid, estrogen and endotoxins were depleting her cellular energy, which is crucial for making energy-intensive decisions.
Her transformation underscores the power of nurturing your health to gain the energy necessary for making significant life changes. Avoiding dietary pitfalls like seed oils played a key role in this journey, enabling her to tap into a newfound capacity for brave decisions — a testament to the profound impact of regaining cellular energy on her ability to navigate life’s choices.
It is my sincere desire and hope that you consider her journey to inspire and empower you to make similar choices in your own life and reclaim the Joy that you deserve. Imagine experiencing the nearly limitless Joy that Ashley has with her 1,000 chickens and four Livestock Guard Dogs below.
From Dr Joseph Mercola:
https://articles.mercola.com/sites/articles/archive/2024/03/11/vegetable-oils-wreck-your-gut.aspx

Yet another example of the principle that if you do the opposite of what the main stream media promote and believe the opposite of what they say then you are going to be right a lot more often than wrong.
In this interview, Christy Sutton, D.C., reviews the dangers of excessive iron. While most doctors look for iron deficiency, few ever pay attention to elevated iron. Sutton is the author of two books, “Genetic Testing: Defining Your Path to a Personalized Health Plan: An Integrative Approach to Optimize Health,” and “The Iron Curse, Is Your Doctor Letting High Iron Destroy Your Health?”
Iron plays an important role in health, especially for children and young adults. Without sufficient iron, you’re not going to be able to form red blood cells and certain proteins in your mitochondria that are responsible for producing energy. On the flip-side, an excess of iron can cause significant damage.
Sutton’s interest in iron has been “lifelong” she says, as she struggled with low iron while her husband has a genetic anomaly that causes him to have elevated iron levels. So, she has personal experience with both ends of the spectrum.
“I have Crohn’s [disease], celiac, and lost part of my small intestine due to Crohn’s when I was 16,” she says. “Because of that, I have to take a bile sequestrant. Then, being menstruating female who’s had a child, low iron has been something that I have been watched very closely for and I had to take iron a lot.
Like a lot of clinicians, when I came into practice, I seemed to be more hyper-focused on people’s problems that were my own problems. I dealt with iron issues. So, I wanted to watch my patients’ iron levels closely. Then I realized, ‘Oh, not everybody is low. A lot of people actually have high iron.’
It wasn’t until I was writing my first book, ‘Genetic Testing: Defining Your Path to a Personalized Health Plan,’ that I discovered the hemochromatosis genes. I realized that my husband had a hemochromatosis gene, and I realized that that was why I kept telling him to donate blood.
His doctor would order iron labs, ferritin, CBC, and he would get elevated iron often, high ferritin. He was developing high liver enzymes and his red blood cells were getting high as well, which is a common issue with people that have too much iron …
He went to a gastroenterologist, because he was trying to figure out why his liver enzymes were high. I thought it was the high iron, but that was presented to the gastroenterologist and dismissed. So, they went down this rabbit hole of misdiagnosing him with autoimmune hepatitis.
Later we went to a hematologist where we figured out he had hereditary hemochromatosis. So, it’s not something that’s particularly difficult to treat. Removing blood, diet supplements, things like that can help.
But once I got really savvy about looking for the genes and the labs combined, I realized that this is a silent epidemic that is not really being talked about. I would tell people, ‘You have a problem with high iron,’ and then they would often go and get a second opinion.
Their second opinion would say, ‘You’re fine. Don’t worry about it,’ which is a common issue where people are getting high iron labs that should warrant more investigation and then they’re just getting dismissed.”
I have beta thalassemia, a hemolytic anemia that results in a high turnover of red blood cells. My red blood cells only live about two months, rather than the normal three months. As a result, my iron tends to accumulate because of the rapid turnover. So, while I do not have the hemochromatosis gene, it results in similar problems. I inherited it from my father, who had a ferritin level close to 1,000 by the time he was diagnosed. Ideally, it should be below 40.
One of the supplements he tried was inositol, also referred to as hexaphosphate or IP-6, but it did nothing. I rapidly came to the conclusion that the supplements typically recommended for high iron are useless and potentially even dangerous, because they prevent you from doing what is really helpful, which is to remove iron through regular phlebotomies.
The most effective way to lower your iron is to donate blood two to four times a year. If losing 10% of your blood in one sitting is problematic for you, then you can remove blood in smaller amounts once a month on the schedule I have listed below. If you have congestive heart failure or severe COPD, you should discuss this with your doctor, but otherwise this is a fairly appropriate recommendation for most.
| Men | Postmenopausal Women | Premenopausal Women |
|---|---|---|
| 150 ml | 100 ml | 50 ml |
As it turns out, Sutton did not include IP-6 in her book, as she couldn’t find any research to back up the claims. She doesn’t dismiss all supplements, however. One of the most helpful, in her view, is curcumin.
“Clinically, I have seen curcumin’s ability to lower iron almost to a fault,” she says. “It’s annoying to me, because I can’t take curcumin for inflammation because it makes me low in iron. But for people that are high in iron or even inflamed with high iron, high ferritin, that’s a great place to start, because curcumin binds to iron.
It also has all of these other wonderful health promoting properties. It’s so good for your brain — it actually helps remove excess iron from the brain and other organs, the heart, liver, spleen.
So, unlike other iron chelators that might be used pharmaceutically, it doesn’t have all these possible negative side effects, but it works very effectively. I mean, I’ve seen it be used in hereditary hemochromatosis patients to lower iron without blood removal … Now, people that have really high iron might need 3 grams a day, which can create diarrhea. So, you have to look at other potentially limiting factors.”
She also recommends taking curcumin with an iron-rich meal, such as shellfish or red meat, to inhibit iron uptake. Other supplements that help bind iron include silymarin, (an extract from milk thistle). It too is very good for hemochromatosis patients, because it lowers iron and helps protect and repair the liver. Another thing that binds to and lowers iron is alpha-lipoic acid. It’s also great for protecting nerves and lowering blood sugar.
“I don’t think silymarin lowers iron quite as much as curcumin, but it’s still a significant way to lower iron,” she says. “The best way to take these — to lower iron — is take them with iron-rich meals. If you want to take them just for medicinal properties but not to lower iron, take them away from iron-rich meals.”
Health Risks Associated With High Iron
The health risks of high iron are manifold and include an elevated risk of skin infections and skin cancer. I suspect high iron may actually be a catalyst when it comes to skin cancer, along with high linoleic acid (LA) intake. LA is oxidized by iron, creating something called lipofuscin, which is basically iron attached to oxidized LA.
A more common term for lipofuscin is liver spots. So, liver spots are a dermal representation of oxidative damage to LA by high iron. Similarly, skin cancer is likely driven by a combination of high LA and high iron. Ancestral LA levels were below 2%. Today, the average is around 25%. If you had normal ancestral levels, you could have higher iron yet not get as much damage.
There are several potential diagnoses related to iron, including iron deficient anemia, copper deficient anemia, iron overload and hereditary hemochromatosis, and getting to the correct diagnosis can be tricky.
“The nice thing is that you can always fall back on labs,” Sutton says. “You don’t want to just use symptoms to guide you, because if you’re using symptoms, then this person is well far down a pathological path that you could have potentially stopped years ago, if not decades before.”
Starting with hereditary hemochromatosis, this is when you have inherited one of three hemochromatosis genes, which causes increased iron absorption by decreasing hepcidin, a liver protein. If you have the hemochromatosis gene, you don’t make as much hepcidin, causing you to absorb more iron.
That can become pathological, because over time, you just keep absorbing more and more iron, until your body finally runs out of places to put it. The first place that gets overloaded is your liver. After that, your body will store the iron in other organs, such as your heart, pancreas, brain, pituitary gland, gonads, ovaries, testes and skin.
Eventually, the iron will go everywhere because the human body has evolved to hold onto as much iron as possible. The only way, really, to lose iron is through blood loss. This is why menstruating women have a lower risk for high iron and a higher risk for low iron.
“Having said that, when you start looking at the hemochromatosis genes, all bets are off, because you’ll see females that have these hemochromatosis genes that develop high iron … you will even see children with the hemochromatosis genes that develop high iron,” Sutton says.
“I discovered that in my colleague’s 5-year-old, where predatory hemochromatosis was causing her to have severe neurological problems. That was a very difficult thing to get through because the hematologist didn’t really want to deal with it.
When you look at labs, hereditary hemochromatosis can look very similar to non-hereditary hemochromatosis, which is where you have high iron but you don’t have one of those hemochromatosis genes.
So, for you, you have more of a non-hereditary secondary hemochromatosis, because you have that thalassemia issue where your red blood cells are breaking and letting all this iron out and then you develop high iron with potentially low red blood cells.
That’s common with thalassemia. Some people, they don’t have a thalassemia gene and they develop high iron without hemochromatosis gene, because they’re just eating a lot of iron-rich foods and they’re not losing iron through menstruation. This is usually men.”
When it comes to lab work, Sutton recommends starting with a full iron panel, a complete blood count (CBC) test, gamma-glutamyl transferase (GGT), and a comprehensive metabolic panel to ensure you have sufficient liver enzymes. Measuring your copper and ceruloplasmin levels can also be helpful.
“The full iron panel has the ferritin, the TIBC [total iron-binding capacity], the UIBC [unsaturated iron-binding capacity], the serum iron and the iron saturation. With hereditary hemochromatosis, you develop high ferritin with a high iron saturation. That combination is hereditary hemochromatosis. So, over 45% iron saturation and high ferritin …
With hereditary hemochromatosis, you’ll see high iron, you’ll see the TIBC go low, the UIBC go low. The serum iron often goes high, and then that ferritin will go high. You’ll often see the liver enzymes go high and it’s common to see the red blood cells, hemoglobin, hematocrit go high.
But that doesn’t always happen. These days, so many are taking testosterone. So, you have to always ask, ‘Are you on testosterone?’ Because that can cause red blood cells, hemoglobin, hematocrit to go high as well …
I always get the GGT as a part of the labs that I order. Occasionally, I will see a high GGT when the AST and ALT, which are the other two liver enzymes, are normal. More often than not, I’ll see a high ALT or high AST. Usually, if they’re not drinking alcohol and they just have high iron, you’re going to see that high ALT.”
Sutton recommends keeping ferritin below 100. Ferritin above 100 means you’re either inflamed, have high iron, or both. Studies referenced in her book suggest that anything over 200 is pathological. The higher your ferritin level, the shorter your lifespan. You’re also more likely to die of a heart attack and cancer.
“I feel like 100 is high enough that I’m not swooping everybody in, but low enough that I’m not leaving stragglers out,” she says. “Now, if somebody has a ferritin over 100 with an iron saturation that is in the 40s or higher, then I’m highly suspicious of a hemochromatosis gene and I immediately want to get those hemochromatosis genes tested.
If they have a hemochromatosis gene, then we know why they’re high on iron and we know where this story is going — and it’s not going to be a pretty picture most likely. Then it’s time to refer to a hematologist … and talk to them about how to get iron lower …
The key is, if you don’t have a hemochromatosis gene, then you need to figure out ‘Why does this person have high iron? Do they have a thalassemia gene? Are they just eating a lot of iron?’ And then, ‘Do they have hemolysis for some unknown reason?’ That’s a non-hereditary hemochromatosis situation.
The treatment is basically the same, other than you want to use more of the supplements, go really heavy on the supplements to lower iron. If you have plenty of red blood cells and hemoglobin, then therapeutic phlebotomy is a wonderful place to start.
A lot of times people don’t because they either have a thalassemia issue where their red blood cells are getting chewed up too quickly, or they have lost so much blood so quickly because their doctors are just trying to get the iron down that they become low in hemoglobin or red blood cells. Rather than waiting for months for that to recover, you could be doing the supplements to lower the iron.”
Sutton’s husband also developed a pituitary tumor that was causing him to have high cortisol (Cushing’s disease). “Ultimately, I think the high iron created a lot of oxidative stress on his pituitary gland,” Sutton says. The only reason he was diagnosed early enough to save him was that they’d been checking his cortisol and DHEA on a regular basis.
“Periodically, they would jump up and then go back down. Then when the hemochromatosis got properly treated and the DHEA was still high, we were like, ‘Why is this happening?’ So we went to the endocrinologist and I said, ‘I’m worried my husband has Cushing’s.’ She was like, ‘He doesn’t have Cushing’s. He doesn’t look like somebody with Cushing’s. His hemoglobin A1C is normal.’
Five months later, he’s having surgery to remove the pituitary tumor. The reason I say that is because for years, he was told, ‘You just need to exercise and lose weight.’ His problem was not exercise. He had a pituitary tumor and hemochromatosis. Hemochromatosis was destroying his liver and his brain and his heart and everything else, and the pituitary tumor was causing him to have high cortisol, which made him look overweight.”
I believe progesterone may be one of the best ways to treat Cushing’s disease, as it very effectively blocks cortisol. Other natural substances that will inhibit cortisol include aspirin, DHEA, pregnenolone, emodin, vitamins A and D, gelatin or glycine, and niacinamide.1
The normal dose for progesterone is 25 to 50 milligrams. For Cushing’s, I would recommend about 300 mg. It’s virtually impossible to overdose on progesterone and there are no downsides to it. One caveat is that you need to administer it correctly to gain the optimal effects.
Avoid creams, pills and suppositories. Instead, mix pharmaceutical grade progesterone with the contents of one natural vitamin E capsule. Mix it with a paperclip or tiny spoon until all the powder is dissolved, then rub it on your gums. Vitamin E is the only natural compound that dissolves progesterone completely. For guidance on how to pick a good vitamin E supplement, see “The Four Hormones Most Adults Need More Of.”
As explained by Sutton, iron deficient anemia is a serious issue. Children born of women with iron-deficient anemia have significantly higher risk of low IQ, ADD, ADHD and other neurological issues that often do not go away with age.
“Many kids suffer from low iron, because they eat a lot of calcium rich foods. Calcium binds to iron, and then you get low in the iron. Maybe they’re picky eaters, they’re growing rapidly. So many kids are not being checked for their iron levels and they’re being diagnosed with ADHD when their problem is actually just low iron, because if you don’t have enough iron, you can’t make dopamine. So, low iron is a serious issue.”
People with iron-deficient anemia will typically have high TIBC and UIBC, as their bodies are trying to mobilize more iron. Serum iron and iron saturation will be low and ferritin will typically be below 30.
“Now, iron deficient anemia is more complicated in many ways because the question is, why are you low in iron?” Sutton says. “There’s so many reasons that you can be low in iron. Are you just not eating enough? Are you not absorbing it? I think the most common reasons that people develop low iron is because they have a GI bleed. They have intestinal malabsorption issues, maybe undiagnosed celiac disease.
There is a gene that can cause you to be more likely to have low iron. I have that gene and that gene actually causes you to make more hepcidin. With iron-deficient anemia you’ll also see low red blood cells sometimes, low hemoglobin and low hematocrit. MCH [mean corpuscular hemoglobin] might get low, MCV [mean corpuscular volume] might get low.”
One common cause for iron-deficient anemia is a deficiency in copper. Paradoxically, lack of copper is also a common cause for iron overload. Sutton explains:
“The reason for that is because copper is necessary for two key enzymes. The first one is called hephaestin and the second one is called ceruloplasmin. Hephaestin is in the lining of the gut, the intestinal lining. Copper is necessary for iron to be absorbed in the gut lining. So, without copper, you will not absorb iron and you will develop iron deficient anemia.
Once iron has been absorbed in the gut lining by hephaestin, it passes it off to ceruloplasmin, which is the second copper-rich enzyme. Ceruloplasmin basically then allows that copper to transfer in and then move throughout the body. So, without ceruloplasmin, iron gets stuck in the tissues. It’ll get stuck in the digestive system, it’ll get stuck in the retina, it’ll get stuck in the brain, it’ll get stuck in the liver.
So, you develop iron overload in the tissues. But eventually, if you’re low in copper long enough, you might then become low in iron, and then you don’t end up with all this extra iron in the tissues. The solution is take copper to fix that problem. That’s the way you solve copper-deficient anemia.
Copper-deficient anemia looks very similar to iron-deficient anemia if you’re looking at the iron panel. You’ll have a high TIBC, high UIBC, low serum iron, low iron saturation, low ferritin. You’ll also potentially see low neutrophils and low white blood cells, because you need copper to have normal immune function as well. So, you might be more at risk for infections.
Then of course you can look at the ceruloplasmin. I don’t find ceruloplasmin to be the easiest lab to look at, because it’s an inflammatory marker … If you’re taking hormones like estrogen or birth control or you’re pregnant or you’re just inflamed or have an infection, ceruloplasmin can jump around and go high.
If you have a low or low-normal ceruloplasmin, and then you take copper and ceruloplasmin goes up, that’s a good sign that you didn’t have enough copper.”
The best way to get iron is through your diet. Shellfish and beef are iron-rich foods with highly absorbable iron. That’s key, because there are two types of iron: heme iron and non-heme iron, the latter of which is not very absorbable. Heme iron is found in animal products while non-heme iron is found in vegetables such as spinach.
“If you’re not eating iron-rich foods like red meat, then you’re more likely to get low in iron if that is something that you struggle with,” Sutton says. “If you struggle with being high in iron, maybe you don’t want to eat as many of those things or maybe you just want to remove blood and supplement accordingly, so that you continue to eat those things.
The form that I like if I’m going to go to a supplement is ferrous peptonate, which I found to be the gentlest on my gut but also get the iron levels up. I really don’t like ferrous sulfate, which is the most common given iron. I don’t think it works very well, and it tends to create a lot of stomach pain. I always have to take my iron with food and sometimes I’ll add copper or vitamin C to it. If I don’t take it with food, it’s really going to upset my stomach.”
To learn more, check out Sutton’s books, “Genetic Testing: Defining Your Path to a Personalized Health Plan: An Integrative Approach to Optimize Health,” and “The Iron Curse, Is Your Doctor Letting High Iron Destroy Your Health?”