
Bill Porter – The Man Who Showed Up

They didn’t just reject him. They made it official.
The State of Oregon typed it up and handed it to him in writing: unemployable. Go home. Accept the benefits. Stop trying.
Bill Porter kept the letter. Then he went looking for a job anyway.
Bill was born in 1932 in San Francisco. The delivery appeared routine. The birth certificate noted no abnormalities. But something had shifted during those final critical minutes — and by the time Bill was a toddler, his parents had a name for it. Cerebral palsy. His muscles fought him constantly. His right hand curled inward. His speech came out slow and thick, difficult for strangers to follow. Walking wasn’t natural. It was a negotiation with his own body, every single day.
His mother, Irene, refused to let that become his story.
She enrolled him in public school. She pushed him. She told him — not gently, but firmly — that his condition was not an excuse. Not once. Not ever.
Still, the world had other ideas.
After his father passed away in the early 1960s, Bill was suddenly without income, without a safety net, and without options. He applied everywhere. Companies turned him away before he could finish a sentence. Some didn’t bother hiding their reasons. And then the State of Oregon made it formal: he was not fit for work. He should stay home.
Bill was asking for door-to-door sales — the most physically punishing job available. On foot. In all weather. Up and down the steep hills of Portland. Every company he approached said no. Including Watkins Incorporated, the oldest direct-sales company in the country.
So Bill went back to Watkins and made them an offer they couldn’t lose.
Give me the worst territory you have — the route nobody wants. I’ll work entirely on commission. You risk nothing. I just need the door opened.
They said yes.
And then Bill Porter got to work.
He was out before 8 every morning, a leather briefcase tucked against his body, steadied with his chin. Seven miles a day. Then seven more. Through Portland winters where ice turned sidewalks into obstacles. Through summer heat that pushed past 90 degrees. He never called in sick. He never asked for a shorter route.
Some doors slammed the moment customers saw him. Others spoke to him loudly and slowly, as though his body’s condition reached his mind too. A few were openly cruel. There were mornings he knocked on 40 doors and walked away with nothing.
He went home. He soaked his feet. He set his alarm for 5:45 a.m.
And he was back at the first door before 8 the next morning.
Weeks passed. Then months. And something quietly remarkable began to happen.
The customers who gave Bill a chance started to realize something: he remembered everything. Not just their orders — Mrs. Henderson takes the small bottle, not the large. Mr. Kimura’s wife just had surgery and needs the gentler soap. He remembered names, preferences, offhand comments from months ago. Details people had forgotten they’d even mentioned.
And then Bill noticed something else.
Many of his customers — elderly women living alone, men recovering from illness, couples who rarely left the house — were lonely. Some hadn’t had a real conversation in days. So Bill started staying a little longer. He asked how they were doing. He listened to the answer. When someone mentioned they needed groceries but couldn’t get out, Bill wrote down the list and brought them back on his return. No charge. No announcement. Just because it was the right thing to do.
That was the product nobody saw in the catalog.
By the 1980s, Bill Porter had become the top-grossing Watkins salesman in the entire United States of America. Not in Oregon. Not in the Pacific Northwest. Number one in the whole country — the man a government office had declared unemployable.
In 1995, The Oregonian ran a feature story on him. It spread nationwide. Reader’s Digest picked it up. ABC’s 20/20 aired a segment on Bill that became one of the most-responded-to stories in the program’s history. In 2002, TNT made a film of his life — Door to Door — with William H. Macy playing Bill and Helen Mirren as his mother.
When reporters asked how he felt about all the attention, Bill always gave the same answer.
“I’m just living a simple life. Who would want to know about my life?”
He genuinely didn’t understand what people found remarkable.
To Bill, he was just doing his job.
He walked his route for nearly six decades. Tens of thousands of miles on a body the world had written off before he turned thirty. He died on December 3, 2013, in Gresham, Oregon, at the age of 81.
The customers he served didn’t remember him because of what he sold them.
They remembered him because he showed up. Every week, without fail, in the rain and the heat and the ice. Because he knew their names. Because he ran their errands. Because he stopped, and he listened, and he made them feel like they mattered.
The disability that was supposed to end his story became the very reason the story couldn’t be forgotten.
Because Bill Porter proved something that no certificate, no rejection letter, and no official document can ever take away:
The world’s verdict on what you cannot do means absolutely nothing compared to what you decide to do anyway.
Soil Remediation

Industrial farms abandon heavily contaminated topsoil — and the industry has never explained why.
But a flawless natural weed already solved this — centuries before the industry existed.
Meet the forgotten phytoremediation method of the Byzantine Empire.
In the 10th century, the Geoponica encyclopedia detailed planting the resilient Bladder Campion.
Its cellular vacuoles actively trap and lock away heavy metals from the soil matrix.
This botanical workhorse literally vacuums toxins directly out of the choked dirt.
Modern experts claim poisoned land must be mechanically excavated at massive expense.
Deploying this plant transforms land from permanently CONTAMINATED to organically EXTRACTED.
Save this before you need it and it is gone from your feed.
They called it primitive. The records proved them wrong. Why did nobody tell you?
Informed Consent…Cholesterol Lowering Statins Are One Of The Most Dangerous Drugs In Today’s Modern World

46% increase in ‘new onset’ Type 2 Diabetes.
For every 30 mg drop in Cholesterol, all cause mortality goes up 22%.
Lowering LDL below 70 mg/dL raises stroke risk 2X.
Lowering Cholesterol Is Dangerous & Harmful…
The Minnesota Coronary Experiment (MCE, 1968-73) showed that for every 30 mg/dL (0.78 mmol/L) decrease in serum cholesterol, resulted in a 22% higher risk of death from any cause.
Lowering LDL Can Be Deadly…
The 2019 study in Neurology Journal entitled, ‘Low-density lipoprotein cholesterol and risk of intracerebral hemorrhage’ stated “when LDL levels are chemically lowered with a statin below 70 mg/dL (brain bleeds) hemorrhagic stroke increases by 2.1 times.”
Statins Cause New Onset Type 2 Diabetes…
In the 2015, 6 year follow-up study of the METSIM cohort, “Participants on statin treatment had a 46% increased risk of type 2 diabetes.”
Statins Do Not Benefit Any Meaningful Longevity…
In the BMJ Open, “The effect of statins on average survival in randomised trials” reports the median postponement of death for primary prevention trials was 3.2 days.”
Common Statins & LDL Lowering Medications…
Rosuvastatin: (Crestor)
Atorvastatin: (Lipitor)
Simvastatin: (Zocor)
Fluvastatin: (Lescol)
Lovastatin: (Mevacor/Altoprev)
Pitavastatin: (Livalo)
Pravastatin: (Pravachol)
Non-Statin Cholesterol Lowering Drugs Causing Similar Side Effects…
Repatha (Evolocumab)
Zetia (Ezetimibe)
Nexletol (Bempodoic Acid)
Serious Adverse Events From Cholesterol Lowering Statins:
Widespread Muscle Pain
Muscle Tearing (Rhabdomyolysis)
Autoimmune Disease (Necrotizing Myopathy)
Aphasia
Dementia & Alzheimer’s Disease
Cancer
Pancreatitis
Liver Inflammation & Damage
Type 2 Diabetes
Depression
Drug Induced Lupus
Parkinson’s Disease
Hemorrhagic Stroke
Lou Gehrig’s Disease (ALS)
Hormone Deficiency
Neurological Damage
Multiple Sclerosis Autoimmune
Fatigue & Weakness
Neuropathy
Heart Failure
Vertigo
Cognitive Impairment
Drug Induced Fibromyalgia
Saturated fat & cholesterol have no effect on CVD outcomes, including heart attacks, strokes, CVD mortality & total mortality.
Heart health is achieved by keeping triglycerides low & HDL high. Both of these are diet controlled. The ratio between the 2 levels should be less than 1.5 which indicates cardiovascular health.
Triglycerides lower quickly when sugar, seed oils, ultra processed foods, artificial ingredients & processed carbs are eliminated from the diet.
HDL can be raised by strength training & consuming animal sourced foods & saturated fats such as beef, bison, venison, eggs, butter, tallow & ghee.
Click to view the video:
https://x.com/ValerieAnne1970/status/2063969298444329098?s=20
Stop Eating These

Lower ‘Biological Age’ Strongly Linked to Brain Protection

Your brain ages based on your internal health, not just your birthday, and when your biological age runs higher than your actual age, your risk of stroke and cognitive decline rises sharply.
Lowering your biological age leads to measurable brain protection, including reduced stroke risk, less structural damage, and better preservation of memory and thinking ability.
Your environment plays a major role in brain aging, with combined exposures like pollution, stress, and social conditions having a far stronger impact than any single risk factor alone.
Brain damage builds gradually through inflammation, poor blood flow, and metabolic stress, which means early changes in your lifestyle directly influence long-term brain health.
Improving metabolism, reducing toxic exposures, staying active, using sunlight wisely, and managing stress work together to slow biological aging and protect your brain over time.
(Tom: I read this and realised the omission, ‘How to work out your biological age’ so I had a conversation with ChatGPT and it directed me to https://checkbioage.com/ where you can enter some results from a recent blood test to get a more accurate assessment than just a lifestyle survey.
Here is the chapter on the subject from my book How To Live The Healthiest Life available at https://howtolivethehealthiestlife.com/)
Finish reading: https://articles.mercola.com/sites/articles/archive/2026/06/09/biological-age-brain-protection.aspx
Charles Schulz and Harriet Glickman

Eleven days after they killed Dr. King, a teacher sat down to force a Black child into America’s most famous comic strip. Harriet Glickman wrote Charles Schulz in 1968 and asked him to put a Black kid in Peanuts, where in eighteen years not one had ever appeared.
He almost said no, afraid that a white man drawing a Black child would look like pity. A hundred million readers, eighteen years, and the whole thing turned on one letter.
Eleven days after Dr. King was killed in Memphis, a schoolteacher in California sat down at her typewriter and wrote a letter to a cartoonist. She did not expect him to write back.
Her name was Harriet Glickman. She was forty-one, a mother of three living in the San Fernando Valley, and that spring she felt as powerless as everyone around her.
The country was coming apart. Cities were burning, the television was wall to wall with funerals, and a teacher in suburban Los Angeles kept asking herself what one ordinary person could possibly do.
She was not an activist.
She was a mother with a typewriter and a feeling she could not shake.
The man she wrote to was Charles Schulz. His comic strip, Peanuts, ran in around a thousand newspapers and reached close to a hundred million readers every week.
Charlie Brown, Lucy, Linus, Snoopy.
Eighteen years of that strip, going back to 1950, and not one of those children was Black.
Glickman had spent her life around children. As a teacher, she had watched something up close that stayed with her.
Black children and white children never saw themselves sitting side by side, not in school in the funny pages, not anywhere a child went looking for his own face.
So she said it plainly on the page. She wrote that since Dr. King’s death she had been asking what she could do about the “vast sea of misunderstanding, hate, fear and violence” that had swallowed the country.
She had actually sent the same idea to several cartoonists. Schulz was the one who wrote back.
That was the first surprise.
His reply was honest in a way that probably stung. He told her he had thought about putting a Black child in the strip, and that the idea frightened him.
Not because of his readers.
He was afraid of getting it wrong.
He worried it would come off like a white man patting Black families on the head, talking down to them. “I don’t know what the solution is,” he wrote, and left it right there.
A lot of people would have folded at that. A polite no from a famous man is an easy place to stop.
But Glickman wrote again, and Schulz answered again, and this time he sounded even more certain it was a mistake. He was sure that whatever he drew would come off as a white man being clumsy about something this raw.
Still she did not let it drop.
She wrote back and asked his permission to do one small thing.
She had no interest in speaking for Black people. So she asked if she could show his letter to some Black friends of hers, parents, and let them answer him in their own words.
Schulz said yes.
One of those friends was a man named Kenneth Kelly. He was a Black father of two young boys, and he was an engineer.
Not just any engineer.
Kelly worked on the Surveyor program, the unmanned American craft that was setting down on the surface of the moon.
Sit with that picture for a second. A Black man helping land a spacecraft on the moon took the time to write a cartoonist about whether a Black child could sit in a comic strip.
Kelly was patient with him. He told Schulz that no Black parent he knew would call the gesture condescending, and that even if a few did, it would be “a small price to pay” for what it would give their children.
What it would give them was not complicated. It was the simple sight of themselves, somewhere inside the ordinary American picture they were shut out of every single day.
Kelly even told him how to do it. Do not make the boy a hero, he suggested, and do not turn him into a lesson.
Just a regular kid, one of the gang, nothing special, simply there.
Years later, Kelly would spend himself fighting housing discrimination in his city. That summer, he changed a comic strip instead.
Another friend and parent, Monica Gunning, wrote to Schulz as well. The letters kept landing on his desk in Northern California, polite and unhurried and impossible to wave off.
All of this was happening while the year kept getting worse. In June, Robert Kennedy was killed in Los Angeles, Glickman’s own city, a few weeks after Kelly mailed his letter.
The country was taking blow after blow.
And in the middle of it, that quiet argument about a comic strip kept moving forward, one letter at a time.
Then, one day that summer, Schulz sent Glickman a short note. He told her to check her newspaper the week of July twenty-ninth, because he had drawn something he thought would please her.
On July 31, 1968, Charlie Brown is standing on a beach, and he has lost his ball in the water. A boy he has never met before wades in and carries it back to him.
The boy’s name is Franklin. The two of them get to talking and build a sandcastle together, two children on a beach on a summer afternoon.
No speech. No halo.
No lecture about brotherhood, just a Black child being kind to Charlie Brown, printed in a thousand papers from coast to coast.
The strip would later show that Franklin’s father was a soldier serving in Vietnam. He was never written as a symbol.
He was somebody’s son.
When Franklin appeared, mail poured into Schulz’s office from all over the country. Most of it said the same simple thing, which was thank you.
It should have ended there, small and sweet. It did not.
When Schulz later drew Franklin in school, he sat him at a desk right in front of Peppermint Patty. A Black child and a white child, learning in the same room.
For one Southern newspaper editor, that was the line. He wrote to Schulz to say he did not mind a Black character, but please do not show the children in school together.
The man could accept Franklin existing in the strip.
He could not accept that child sharing a desk with a white girl.
This was 1968. Black children were walking into newly integrated schools behind federal marshals, and a grown man was objecting to a cartoon doing the very same thing.
Schulz had a decision to make, and he made it without any noise. Years later, asked what he had done about that complaint over the classroom, he gave a short answer.
It was five words. “I didn’t even answer him.”
He just kept drawing the two of them at the same desk.
Far off in Philadelphia, a six-year-old Black boy watched Franklin appear with no idea of the fight behind him. His name was Robb Armstrong.
That year had already taken something from him. His older brother had died thirty days before Franklin first turned up on that beach.
Thirty days.
A boy loses his brother, and a month later a new face shows up in the comics page he reads on the living room floor.
So here was a child who already knew the shape of a hole in a family. And then, right inside that grief, a Black kid walked into his favorite comic strip.
Robb looked at Franklin and thought one thing. “That’s like me.”
He had already told his mother, at three years old, that he was going to be a cartoonist.
Now he had proof there was room for him.
A Black boy could belong on the funny pages, because one already did.
That child grew up to become exactly what he had promised. Robb Armstrong created JumpStart, one of the most widely syndicated Black comic strips in the country.
And here is where the story closes a circle no one could have planned. Franklin, through all those decades, never had a last name.
In the 1990s, Charles Schulz picked up the phone and called Robb Armstrong. A special was in the works, every character needed a full name, and Schulz had just realized Franklin did not have one.
So he asked the grown man, the one who had once been that grieving six-year-old, whether he could borrow his name. Robb said yes right away.
That is why the first Black character in Peanuts is named Franklin Armstrong.
Armstrong called it the highest respect a person could be shown.
About the man who reached a lonely kid through a comic strip, he said it simply, “He inspired a kid.”
Harriet Glickman lived to be ninety-three. She died in March of 2020, in the same Sherman Oaks house where she had typed that letter more than fifty years earlier.
The letter outlived her. It rests now in the Charles M. Schulz Museum, the real page, her real words, dated eleven days after Dr. King was killed.
You can stand in front of it today, behind glass, and read the date typed across the top. April 15, 1968, mailed by a woman who was certain no one was listening.
Professors Scolyer, Allen, McLaws and Johnston
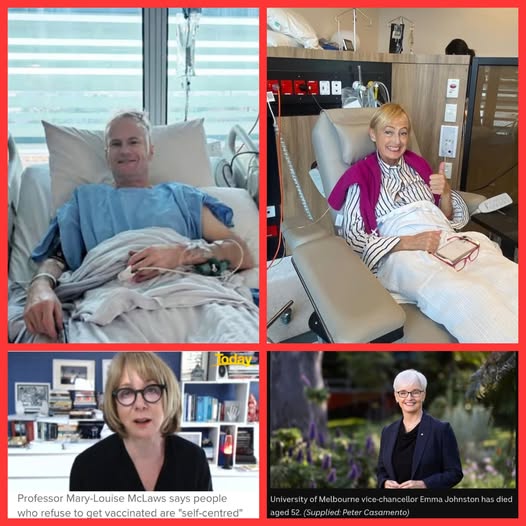
A tale of four Australians – what do Professors Scolyer, Allen, McLaws and Johnston have in common?
All have Dr. before their names and AO after.
All have died from turbo cancer which was most likely caused by the covid vaccine that they promoted.
All didn’t need the vaccine but chose to have it to advance their careers.
All knew that mandates are the tools of bullies, criminals and dictators.
All lived by the system, advanced by the system and eventually killed by the system.
All will be remembered for not speaking up when they could have helped stopped the madness
Vadim Zeland

(Tom: This aligns with what I understand, that when we descend from making things happen by lightly deciding they will happen down to using energy to make them happen we are less likely to obtain the desired result.)
Somewhere in Russia, there is a man who does not want to be found.
Not because he is hiding from trouble. Not because he is ashamed of what he has written. But because he genuinely believes that who he is has nothing to do with whether his ideas are true — and that making himself the story would only get in the way.
When readers ask him “Who are you, Vadim Zeland?” he gives the same answer every time: “I’m no one special.” Wemoral
No photographs. No interviews. No stage appearances. No social media presence. Just books — released quietly into the world — and then silence.
He has said: “My biography cannot and should not be of any interest. To transmit this knowledge without personal distortions, I really ought to be nobody. Just an empty vessel.” Wemoral
This is either profound humility or masterful mystique. Possibly both.
What is known about him is this: before the collapse of the Soviet Union, he did research in quantum physics. Afterward, he worked in computer technology. Then, in the early 2000s, he began writing. Wemoral
The books came out in Russia starting around 2004. They spread first through word of mouth — friend telling friend, stranger telling stranger on early internet forums. No advertising. No celebrity endorsements. No famous face attached.
Just readers saying, quietly, to anyone who would listen: “Something about this is different. Try it.”
The series is called Reality Transurfing. And the central idea — stripped of its more contested theoretical packaging — goes like this:
Most people approach what they want in life the wrong way. They strain toward it. They obsess. They assign it enormous importance. They pour so much desperate energy into wanting something that the wanting itself becomes the obstacle. Like gripping water in a clenched fist: the harder you squeeze, the faster it escapes.
Zeland’s proposal is a fundamental shift in approach.
Stop making your goals so desperately important. Choose what you want clearly, calmly, with quiet confidence — as if you are selecting something from a menu rather than clawing toward it. Align your inner state with the version of yourself who already has the thing you’re reaching for. Stop straining. Start moving.
He frames this through the language of quantum physics and parallel possibilities — describing reality as a vast field of branching variants, and your life as something you navigate by shifting your inner frequency rather than forcing external outcomes.
Here is where honest reporting matters: physicists and scientists have consistently pointed out that Zeland’s use of quantum physics terminology does not accurately represent how quantum mechanics actually works. Quantum effects operate at subatomic scales — they do not function the way self-help writers often describe them. This is a legitimate and important criticism that serious readers of Transurfing should know. All That’s Interesting
Zeland himself, to his credit, has acknowledged this. He says the theoretical model is a framework — a way of thinking — not a scientific claim. He has stated clearly: “The use of the techniques is not dependent on the acceptance of his theoretical model.” You don’t have to believe the physics framing. You just have to try the practices. ABC News
And the practices — stripped of the cosmological scaffolding — are recognizable.
Reduce the anxious importance you attach to outcomes. Listen to what you actually want rather than what you think you should want. Stop being swept along by other people’s ideas of success. Move toward your goals from a place of calm intention rather than desperate striving.
These ideas appear in Buddhist philosophy. In Stoicism. In modern cognitive behavioral therapy. In various contemplative traditions going back centuries. Zeland acknowledges the overlaps openly and without defensiveness.
What he brought to them was a specific, practical, systematic framework — written in plain language by someone who described himself as an ordinary person who had, by his own admission, spent most of his life doing everything wrong.
“All my life I had practiced anti-Transurfing,” he once said. “I had done everything just the wrong way. A clever man learns from other people’s mistakes, but a fool always learns from his own ones. In this sense I had been a headstrong fool.” NBC News
There is something disarming about that. No guru claiming enlightenment. No teacher presenting himself as someone who arrived. Just a man who made a mess of his life, figured some things out, and wrote them down.
The books spread. Slowly at first, then faster. Online communities formed — in Russian, then in English, then in dozens of languages — where ordinary people shared their experiences with the practices. The testimonials that fill these communities are anecdotal and unverified. They cannot be taken as scientific evidence.
But they keep coming. Year after year, in community after community, the same kinds of reports appear: a goal pursued desperately for years suddenly moved forward when the desperate pursuit stopped. A relationship that had been stuck shifted when the straining stopped. Opportunities arrived when the grasping relaxed.
Whether these outcomes have anything to do with Zeland’s framework, or whether they reflect the well-documented psychological effects of reducing anxiety and obsessive thinking — effects that mainstream psychology also supports — is genuinely impossible to know from testimonials alone.
The man himself does not claim to know the answer. He says only: try it. Watch what happens.
He remains hidden. No empire. No disciples gathered around a guru. No course selling for thousands. Just the books, just the ideas, just the quiet persistence of millions of ordinary readers who found something useful and passed it on.
Twenty years after the first book appeared in Russia, the conversation continues — in forums and reading groups and comment threads across dozens of languages — between people who have never met and likely never will, connected only by a set of ideas released into the world by a man who insists he is nobody.
Maybe the framework describes something true about reality. Maybe it found a modern language for ancient wisdom. Maybe the practices work for entirely different reasons than the author describes. Maybe the answer is some mixture of all three.
What is true is this: the ideas ask something genuinely difficult of the people who try them. Not to want less. Not to care less. But to hold what they want lightly — with intention rather than desperation, with direction rather than strain.
In a world that constantly tells you to want harder, push harder, force harder — that particular message is quiet and strange and surprisingly hard to find.
Which may be exactly why, twenty years later, people are still passing it along.
“Want what you want. Want it lightly. See what slides toward you.”
Charlie and Nita
Old Man Goes To Visit His Elephant After 15 Yrs…

Click to view the video: https://amazingpandph.com/elephant-best-reunion
